
www.flinturology.com
Urology Services, Inc.
G-1121 West Hill Rd.
Flint, Michigan 48507
Tel: 810.232.8888
Fax: 810.232.9190
Email: jbauer@flinturology.com
[map]
 |
John J. Bauer, M.D.
www.flinturology.com Urology Services, Inc.
|
BPH (Benign Prostatic Hypertrophy)
BPH or Benign Prostatic Hyperplasia is really a misnomer. The prostate itself does not actually enlarge, but rather there is a growth of a benign tumor or adenoma, which obstructs the flow of urine. The prostate sits at the outlet to the bladder, much like a donut. Urine flows through the center of this gland. If the center becomes obstructed (much like the hole in the donut getting smaller), then the patient experiences difficulty with voiding. A rectal exam feels the outside of the prostate (much like feeling the outside of the donut) and although the prostate is often enlarged rectally, it is the narrowing of the hole in the center, which causes symptoms. Thus, some patients will be told that their prostate is large, yet they have no symptoms; while other patients will have a prostate on rectal exam which feels small, yet they have symptoms.
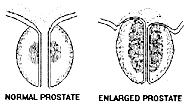
The prostate is composed of three tissue types: fibrous tissue, approximately 33-50%; muscular tissues, approximately 25-33%; and glandular tissue, approximately 25-33% of the gland. As the prostate enlarges, the muscular component tends to contract and causes the outlet to narrow, resulting in some of the symptoms of poor urination. What causes the prostate to develop an adenoma is not fully understood, but the glandular component appears to be, at least in part, under hormonal influence. Male hormone, testosterone, is produced in the testicles. This hormone is taken up by the prostate cells and converted into another male hormone called dihydrotestosterone or DHT. It is this hormone, which is needed to cause the glandular component to enlarge.
The mainstay of treatment of BPH has been surgical removal of the enlarged portion of the prostate, either by open surgery or by transurethral resection of the gland (TURP). In recent years, both surgical and medical therapies have been changing the way we treat BPH. Although some of the treatments are experimental, some alternative ways to treating BPH are presently available.
Surgically, balloon dilatation of the prostate still has a place in a very select group of patients. Its long-term relief of symptoms, however, is poor and almost all patients so treated will return with their prior symptoms within one year of treatment. The placement of a permanent wire stent inside the urethra at the level of the prostate holds some promise, but the long term effects of having a permanent wire mesh or foreign body left in the urethra is unknown, although in Europe, some have been in place for more than five years. Hyperthermia and thermotherapy, mechanisms of "cooking" the prostate, are also being studied and selectively used throughout the country. They, however, either require multiple treatments or a catheter after treatment for a week or longer.
The usual surgical therapy is a TURP (TransUrethral Resection of the Prostate) in which an instrument is inserted through the urethra while under anesthesia and the obstructing prostatic tissue is cut or resected away using a high frequency cutting loop.
Using a LASER as the cutting tool, no tissue is removed, but rather, the prostate tissue is "cooked" by the high intensity light of the laser. This tissue will slough off or disintegrate in the weeks after surgery.
TUVP (TransUrethral Vaporization of the Prostate) is done very much like a TURP. The significant difference is that tissue is vaporized (destroyed) rather than resected (cut away). This has some of the advantages of a TURP and LASER but also fewer side effects of both procedures.
Medically, the treatment of BPH to relieve symptoms has been aimed at two components of the tissue, which cause symptoms: namely, the muscular and glandular tissue. The contraction of the muscular tissue is through the so-called sympathetic nervous system. Specifically, it is stimulated through nerve fibers called alpha-1-fibers. There are a number of medicines available to block the firing of these nerves and prevent the muscle tissue from contracting. The two most commonly used are terazosin (Hytrin) and doxazosin (Cardura). Both of these medications can be taken once daily and both of these medications may cause some dizziness or lightheadedness upon standing up. This side effect usually goes away within the first few days of starting the medicine. Another medication aimed at causing shrinkage of the glandular component is called Finasteride (Proscar). It is a very well tolerated drug with its only side effect being impotency in about 3% of patients. It usually tales at least several months or longer before improvement in urination is noticed.
There are differences in the surgery and post-operative course. The following areas of major differences are:
| PROCEDURE: | Laser | TURP | TUVP |
|---|---|---|---|
| Sexual Activity: | No Restrictions | No Restrictions | No Restrictions |
| Pain after surgery: | Very little | Very little | Very little |
| Hospital stay: | 1 day/ Overnight | 2 - 3 days | 1 day/ Overnight |
| Catheter: | 1 - 3 weeks | 2 - 3 days | Less than 1 day |
| Home with catheter: | Yes | No | Less than 1 day |
| Bleeding at surgery: | None/very little | Up to 1 pint | None/very little |
| Need blood transfusion: | No | Rarely | No |
| Post of urgency to void: | Up to 3 months | About 1 week | About 1 week |
| Retrograde ejaculation: | 10-15 % | 90 % | 90 % |
| Impotency: | 1 % | 2-3 % | 1 % |
| Incontinence post-op: | Less than 1 % | Less than 1 % | Less than 1 % |
| Diet post-op: | No restrictions | No restrictions | No restrictions |
| Restrictions in lifting, etc.: | No restrictions | 6 weeks | No restrictions |
| Pathology tissue available: | No | Yes | No |
All medications have the drawback of requiring lifelong commitment, as the symptoms will return if the drug(s) is discontinued. The combination of both Proscar and an alpha- blocking agent may give better relief of symptoms than either drug alone. Additionally, surgery can still be performed if the drug(s) does not work, is not tolerated, or the patient chooses surgery in order to stop medication.
As you can see, we now have many choices to make in regard to the treatment of BPH. Sometimes, medication is the preferred treatment and sometimes surgery is the preferred treatment. You should discuss this, along with the various treatment options available, with your doctor.