
www.flinturology.com
Urology Services, Inc.
G-1121 West Hill Rd.
Flint, Michigan 48507
Tel: 810.232.8888
Fax: 810.232.9190
Email: jbauer@flinturology.com
[map]
 |
John J. Bauer, M.D.
www.flinturology.com Urology Services, Inc.
|
Orchitis (Testicular Infection and Pain)
John J. Bauer, MD, Urologist
Orchitis is a term used to describe inflammation of the testicle. The testicle is part of the male anatomy, a picture of which is shown. The scrotum, or sac, contains a testicle of each side. The testicle has two functions. It makes testosterone, the male hormone, which is absorbed into the blood stream. It also makes sperm, which travels from the testicle into a series of tubes, which collectively form the epididymis. The epididymis sits to the side and in the back of the testis. Sperm leaves the epididymis by way of the vas deferens (this is the tube that is divided during a vasectomy), which travels to join the seminal vesicles and prostate. Sperm mixes with fluid from the seminal vesicles and prostate to produce the semen, the fluid that comes out from the penis at the time of ejaculation.
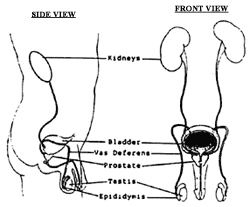
Inflammation of the testicle can occur due to a variety of causes, some of which include urinary infection, viral illness elsewhere in the body, minor physical trauma and reaction to medication. In many cases, the exact cause of an episode of orchitis may not be identified. During examination, the physician checks to make sure other problems are not present which can also cause scrotal pain, such as testicular tumor, hernia, or varicoceole. In some cases, a scrotal ultrasound may be recommended.
Orchitis is typically treated with hot sitz baths, scrotal support, anti-inflammatory medication and occasionally antibiotics. Sitting in a warm tub for 20-minutes a day helps lessen inflammation. Scrotal support, with an athletic supporter or tight jockey style underwear, lessens the tension on the spermatic cord. Anti-inflammatory medication, such as ibuprofen (Advil or Nuprin) at doses of 400-600 mg, 3 times a day can provide pain relief and reduce swelling. Antibiotics are to be used if directed by your doctor. Orchitis may take 2-4 weeks to resolve. If symptoms persist beyond that, re-examination is indicated. Occasionally Orchitis becomes chronic in nature. Treatment of this condition is more difficult. Sometimes a " block" of the spermatic cord is carried out by injecting a mixture of novocaine and cortisone into the groin area. Rarely, surgical removal of the testicle may be necessary (a procedure called orchiectomy).
Chronic Orchitis
In most cases, Acute and the bacterial varieties of Orchitis can be treated very effectively and most men can be relieved of their symptoms. However, if the pain does not respond to these treatments it may be the first encounter with a chronic pain syndrome or myofascial syndrome. These syndromes occur in both male and females. Chronic Low Back Pain (CLBP) occurs in both the sexes. Chronic pelvic pain syndrome and pelvic inflammatory disease (PID) in females is well known. Males also have these syndromes, however, are not as well known to the public. Chronic pain syndromes of the prostate, epididymis and the testicles are some of the male specific myofascial syndromes. These chronic pain syndromes are very difficult to treat symptomatically and they are rarely cured. The patient must be reassured that they do not have a disease process that will end in their demise. A physician must especially reassure the patient that the condition is not caused by a cancer of the specified organ. If initial attempts to treat the pain have failed, the patient must be educated on the disease entity and made aware of the chronicity of the disease. They must realize that they now have a new baseline of pain that is considered normal for them. Any other acute increase in the pain must be treated as an Acute on Chronic disease.
In the past, patients with this disease entity received the proverbial ?million dollar? work-up and unsuccessful surgery. A comprehensive study completed on young soldiers in the military suggests that minimal diagnostic tests and interventions are required. All patients with the disease should have a History and Physical, urine analysis and culture, general labs and a scrotal ultrasound. A multidisciplinary approach with the urologist and the anesthesia/pain clinic environment is necessary to devise a pain management plan that minimizes the symptoms as much as possible.
Treatment
Unfortunately, the treatment of the patient with chronic pain is difficult, frustrating and lengthy for the physician and patient. It is important to identify these patients early, and to eliminate the old and ineffectual diagnoses and treatments. The best treatment for chronic orchalgia is a multidisciplinary approach using the pain management clinic.
Many useful therapeutic techniques involve sensory modification, which can be accomplished through biofeedback training or with counterirritant therapy. The transcutaneous electrical nerve stimulator (TENS) has been helpful in some patients. The mechanism of effect is not understood and could be due to a placebo effect. However, a short course of 1-3 months of TENS is not harmful and could potentially be helpful. In patients with Low Back Pain, up to 85% of patients state that there is some benefit in decreasing the severity of their pain. The only contraindication to TENS is if the patient has a cardiac pacemaker.
While the association of depression and chronic pain is unclear, many patients with chronic pain syndromes will improve on a trial of low dose anti-depressants. Response rates of 44-70% have been reported for patients with Low Back Pain. It is important to start on a low dose at bedtime and titrate to the patients response. This decreases the common side effects of sedation and disorientation. Doxepin (Sinequan) and Amytriptyline (Elavil) appear to have an advantage over other tri-cyclic anti-depressants. They enhance the serotonin reuptake blockade that is involved in pain pathways.
Some times spermatic chord, ilioinguinal, iliohypogastric, and genitofemoral blocks can be beneficial if there has been some sort of damage or irritation to these nerves.
The most important fact is that the physician and patient must learn to develop the best coping strategy for this disease entity, since conventional medical interventions are not that successful in ameliorating the pain.