
www.flinturology.com
Urology Services, Inc.
G-1121 West Hill Rd.
Flint, Michigan 48507
Tel: 810.232.8888
Fax: 810.232.9190
Email: jbauer@flinturology.com
[map]
 |
John J. Bauer, M.D.
www.flinturology.com Urology Services, Inc.
|
Prostatitis
John J. Bauer, MD, Urologist
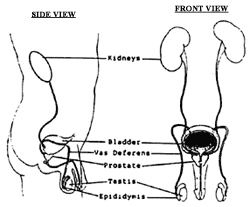
Prostatitis is a term used to describe inflammatory and infectious conditions of the prostate. The prostate is a gland, which is part of the reproductive system that is closely associated with the urinary tract. The urinary system begins with the kidneys, which sit high up in the back. The kidneys filter the blood, take out the excess fluid and waste products, and form the urine. Urine once formed in the kidney travels through a tube on each side called the ureter down to the bladder. The bladder sits in the lower part of the abdomen. The bladder stores the urine until full and then empties the urine to the outside through the urethra, which is the urinary channel that runs through the penis. The prostate wraps around the urethra at the junction of the bladder and the urethra.
As noted above, the prostate is part of the reproductive system. The reproductive system begins with the testicles, which are in the scrotum. They make the sperm, which is carried through a tube on each side called the vas deferens (this is what is divided when a person has a vasectomy). The sperm comes through the vas deferens and mixes with the fluid from the seminal vesicles and prostate to form the semen. The semen is the fluid, which comes out at the time of ejaculation. The prostate makes a portion of the fluid that forms the semen.
Prostatitis is the term used to describe inflammation in the prostate. Acute prostatitis refers to the sudden onset of infection within the prostate gland. It often occurs in association with high fever and typically responds well to antibiotic treatment. Chronic prostatitis refers to ongoing smoldering infection or inflammation of the prostate gland. Prostatodynia refers to pain and discomfort originating in the prostate gland, which is not associated with infection. Symptoms of prostatitis can include lower abdominal or pelvic ache and a sense of discomfort in the testicles or in the rectal area. Pain may also be present in the area behind the scrotum and in front of the rectum. Sometimes there can be an uncomfortable sensation in this area that occurs while sitting. There can even be a sensation of "sitting on a golf ball". Because the prostate wraps around the urethra, urinary symptoms may be present as well. These can include urinary frequency (the need to urinate more often) urgency (the need to urinate as soon as one gets the urge) and nocturia (the need to urinate frequently at night). Burning and stinging with urination may be present as well.
The physical examination begins with inspection of the abdomen and groin area. Then a digital rectal examination is done to feel the surface of the prostate. The physician inserts a gloved finger into the rectal area to feel the prostate to make sure there are not any abnormalities such as prostate cancer. On some occasions the prostate may be "massaged" which means mild pressure is applied while examining the prostate to express prostatic fluid into the urethra. Occasionally, this fluid comes out from the tip of the penis. Alternatively, the patient may be asked to void after the examination to wash out this fluid with the urine. These samples can be inspected under the microscope to determine if inflammatory cells are present. As part of the examination a PSA is often done. This is a blood test done to check for prostatic cancer.
A combination of therapies is used to treat prostatitis. Key components of treatment include anti-inflammatory medication, hot baths and a special diet. Anti-inflammatory medication such as Advil or Nuprin is used to address the inflammatory component. The typical dose is 400 to 600 mgs three times a day. Soaking in a hot bath for 20 minutes a day is important. The warm moist heat helps resolve the inflammatory changes, which occur with prostatitis. Additionally, a special diet may be recommended to avoid foods and beverages, which are irritants to the urinary system. A separate dietary list is available which indicates foods that can cause irritation to the bladder and prostate. Eating foods in the "foods to avoid" column does not pose a threat to the patient's health. However, after eating these foods one may notice that symptoms are exacerbated. The patient then needs to choose between avoiding the foods he may want to eat or putting up with the symptoms that they cause. The final part of treatment may include antibiotic therapy. Different antibiotics are available for treating infection within the prostate. Some of the commonly used antibiotics include Ciprofloxacin, Floxin, Levofloxacin, Doxycycline, Bactrim and Geocillin. It should be noted that using antibiotics alone in the absence of the above three treatments is usually not effective. Antibiotics alone do not typically resolve the problem.
In some cases, prostatitis is associated with spasm of the outer muscular coat of the prostate and the muscles of the pelvic floor. In this case, treatment with medication known as an alpha-blocker can improve symptoms. The two most commonly used alpha-blockers are Cardura and Hytrin. These medications are typically taken once a day at bedtime. Side effects can include drowsiness 1-2 hours after taking the medication, nasal stuffiness and occasionally light-headedness. Some patients notice a favorable improvement in urinary flow when treated with an alpha-blocker. The natural history of prostatitis is that it recurs intermittently over time. However, it does not pose a long-term risk to one's health. It does not lead to kidney problems or prostate cancer. The primary goal of evaluation is to confirm. that the findings are consistent with chronic prostatitis or prostatodynia and to exclude other possible causes of the above symptoms. Once the diagnosis is confirmed, then the main goal is symptom control. The key components of symptom control include anti-inflammatory medication, hot baths and dietary avoidance. Antibiotics are used on an as needed basis.