
www.flinturology.com
Urology Services, Inc.
G-1121 West Hill Rd.
Flint, Michigan 48507
Tel: 810.232.8888
Fax: 810.232.9190
Email: jbauer@flinturology.com
[map]
 |
John J. Bauer, M.D.
www.flinturology.com Urology Services, Inc.
|
Prostate Cancer and Prostate Ultrasound
John J. Bauer, MD, Urologist
Prostate cancer is the most common type of cancer in adult men. The prostate is a gland, which is part of the reproductive system. It makes a portion of the semen, which is the fluid that comes out at the time of ejaculation. The prostate wraps around the urethra, which is the urinary channel that drains urine from the bladder to the outside through the penis. The prostate begins to enlarge in a benign or non-cancerous fashion in almost all men beginning at the age of 40. As it does, it can compress the urethra and cause a change in the pattern of urination. While normal growth of the prostate affects most men, approximately 1 out of 11 men will develop cancer of the prostate. The number of cases of prostate cancer had been increasing steadily over the last several years. In the past, the best way to test for prostate cancer was with a digital rectal examination. This is an exam carried out by a doctor where a gloved finger is inserted into the rectum to palpate the prostate for abnormalities that may suggest the presence of cancer.
Since the early 1990's, a blood test called PSA has been available to help determine if prostatic cancer is present. PSA stands for prostate specific antigen, which is a protein-like substance manufactured only in the prostate. The normal range for PSA is between 0 and 4. When the value is elevated above 4, it may be an early warning sign that prostatic cancer is present. Currently, many doctors are checking the PSA on a regular basis. If elevated, further evaluation may be indicated.
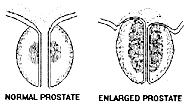
PSA maybe elevated due to BPH, prostatitis or prostatic cancer. One of the most common causes is BPH, benign prostatic hyperplasia, which is the normal enlargement of the prostate that occurs in most men once they reach the age of 40. Non-specific inflammation of the prostate, or prostatitis, is another common cause of PSA elevation.
With an elevated PSA, the next step depends on the degree of elevation. If there is only minimal elevation, we may recommend regular periodic digital rectal examinations of the prostate in association with repeat measurements of the PSA. If the elevation increases over time, further studies are indicated. Alternatively, we may recommend an assessment of the prostate with transrectal ultrasound.
Transrectal ultrasound of the prostate is an imaging technique that provides a complete view of the prostate, allowing visualization of areas, which cannot be felt on a digital rectal examination. Prostate ultrasound is carried out by inserting a small probe into the rectum, which then takes sonographic pictures of the prostate. This is a simple office procedure that is similar to the rectal exam. At the time of the ultrasound, biopsy can be carried out under ultrasound visualization to allow accurate placement of the biopsy needle. Needle biopsy of the prostate is a relatively simple procedure that is similar to having a blood sample drawn from the arm. Complications that can develop after biopsy of the prostate include bleeding and infection, both of which are relatively rare. To minimize the risk of bleeding, patients are instructed to stop all aspirin or aspirin like compounds seven to ten days prior to the procedure. Patients who are taking a blood thinner (i.e. Coumadin) need to stop the medication five days prior to the procedure. To minimize the risk of infection, preventive antibiotics are given the day before, the day of and the day after the procedure. A Fleets enema is usually given the day of the procedure to empty the rectal area.
For patients who undergo ultrasound and biopsy and have benign findings, we recommend careful, ongoing follow up. Patients should have a follow up digital rectal exam and PSA in three to six months after their procedure and at regular six-month intervals thereafter. In some cases even closer follow up may be recommended. As experience with PSA has accumulated over time, further concepts have developed to increase its usefulness. An important feature of PSA appears to be its rate of change over time, referred to as "PSA velocity". For those men with BPH or prostatitis, the PSA may vary by several points a year but it tends to stay in the same range over time. For those men with prostatic cancer, the PSA tends to have a steady rise and the levels can increase by as much as 50 to 100% on a yearly basis.
The level of PSA can also be correlated to the size of the prostate. The "PSA density" is the value of PSA divided by the size of the prostate measured at the time of prostate ultrasound. If the level of PSA is higher than expected for that size prostate, then there may be an increased possibility that prostate cancer may be present. Another variation of PSA testing is known as "free versus total" PSA. A portion of the PSA in the bloodstream is bound to albumin, and the remainder is unbound or "free". The ratio of the free versus total PSA may be useful to help determine if PSA elevation is due to BPH or prostatic cancer.
Finally, different PSA levels have been established for different age groups. The current normal ranges for PSA according to age are as follows:
|
AGE
41-50 51-60 61-70 over 70 |
PSA RANGE
0.0-2.5 less than 3.5 less than 4.5 less than 6.5 |
We have been doing transrectal ultrasound since 1991. This has led to the diagnosis of prostatic cancer in many of our patients. The encouraging news is that many of these prostate cancers tend to be diagnosed at an early stage, when they are still confined within the prostate and have not spread. Prostatic cancer is most curable at this stage. In the past, prostatic malignancies were typically diagnosed once they had already spread from the prostate, in which case treatment was less effective.
Our current recommendation is that all men over the age of 50 have a digital rectal examination and PSA test on a yearly basis. If an abnormality is detected in either instance, further evaluation with transrectal ultrasound imaging can be carried out.