
www.flinturology.com
Urology Services, Inc.
G-1121 West Hill Rd.
Flint, Michigan 48507
Tel: 810.232.8888
Fax: 810.232.9190
Email: jbauer@flinturology.com
[map]
 |
John J. Bauer, M.D.
www.flinturology.com Urology Services, Inc.
|
VASECTOMY
General information about the surgery
[For complete vasectomy surgery details, go to Vasectomy Details.]
An ever increasing number of men and women are seeking protection from unwanted pregnancies. Varieties of temporary or permanent birth control measures are available, and the choice depends on one?s own beliefs, values, and understanding of each method?s advantages or disadvantages. Physical and emotional aspects of these methods have far-reaching consequences. Each couple must carefully consider the alternatives and inform themselves completely. Your physician is very important in assisting you in making this decision.
For men, the most common permanent sterilization method is vasectomy, which is the surgical interruption of the sperm-carrying tubes or vas deferens. Sperm are effectively blocked from reaching the urethra. To be sterilized means being unable to father children. Approximately 500,000 men per year have a vasectomy in physician?s offices, hospitals and outpatient clinics.
Despite the common occurrence of vasectomy, many questions, myths, and concerns still exist. This document is designed to answer these questions, relieve concerns, and to provide factual information about a vasectomy. Benefits, consequences and helpful instructions about this procedure are also included. It is intended as a supplement to physician education and counseling efforts.
A study of the vas deferens anatomy, function and scrotum relationships is vital for a complete understanding of vasectomy. The vas deferens or "cord" as it is commonly called is a muscular tube with an inner canal. It is the size and shape of a pipe cleaner and is located in the back part of the scrotum. It starts at the lower end of the epididymis, which is located behind the testicle and passes through the scrotum and groin into the lower abdomen, then descends to the prostate where it terminates. It is joined by the duct from the seminal vesicle just before entering into the prostate and together they are known as the ejaculatory duct. During the passage of the vas deferens through the scrotum and groin, the vas is surrounded by blood vessels, lymph vessels and nerves. Sperm are produced in the testicle, mature in the epididymis, and travel along the vas until they reach the ejaculatory duct and seminal vesicles where they are stored until time of ejaculation. When the nutrients and fluid from the prostate and seminal vesicle join sperm, the mixture is known as semen. At the time of ejaculation, contractions of the seminal vesicle and prostate force the semen into the prostatic urethra and then outside via the penis.
Five aspects of vasectomy need further explanation.
Men are assuming more responsibility in birth control decisions and in choosing the method of sterilization. Despite an abundance of information on this subject, questions and concerns are common and normal because of the conflicting information from a variety of sources. The most common questions are answered with the help of current scientific knowledge and the personal experience of men who have had a vasectomy.
Q. What advantages does vasectomy have over other forms of birth control?
A.
Q. Is my manhood affected by vasectomy?
A. There is no change in sexual performance. The ability to have an erection and satisfactory intercourse with orgasm and ejaculation is maintained. Since sperm occupies only a small portion of semen, the volume of ejaculation is almost the same. Male hormones do not flow through the vas. They continue to be produced by the testes and enter the circulation through the blood vessels, which are not interrupted by vasectomy. Some couples say that their sex life is improved because the fear of pregnancy is gone.
Q. After vasectomy what happens to sperm produced by the testicles?
A. Since sperm cannot pass the blocked vas, the cells disintegrate and are absorbed by the body just as other cells in the body are broken down and replaced.
Q. If I change my mind, can I have the tubes spliced back together again?
A. Yes. An operation, vasovasostomy, is available for this purpose. The scarring at the ends of the vas are removed and with the help of an operating microscope the ends are rejoined with fine suture material. While the results are encouraging and constantly improving, vasectomy should be considered a permanent procedure until the success rate of vasovasostomy reaches 100%. The time delay between vasectomy and reversal is also a factor in success or failure.
Q. I have heard a lot about potential health hazards because of vasectomy. Am I to be concerned?
A. No, overall, the weight of the evidence suggests that there is no consistent association between vasectomy and prostate cancer, testicular cancer, or heart disease.
Medical precautions
Certain medical conditions influence the success of vasectomy. Should any of the following apply to you, notify your physician in advance of vasectomy.
Shaving the scrotum and penis
Shave your lower portion of your penis and the entire scrotum. Do not use an electrical razor, hair remover or aftershave on the scrotum. Bathe after shaving and remove any loose hairs from the scrotum and penis. Wear clean underwear for the vasectomy.
Athletic supporter
Bring a suitable size athletic supporter or suspensory with you. If none are available, wear jockey type undershorts or briefs.
Consent form
If given to you to take home prior to vasectomy, bring the signed document with you.
Meal
A light snack or liquids are preferable to any heavy food before vasectomy.
Travel to appointment
Arrange to have someone drive you home.
Come to the physicians office in a relaxed frame of mind. Being "uptight" can cause the scrotum muscles to draw the testicles close to the abdomen and make it more difficult to grasp the vas. You should have shaved and cleansed the scrotum prior to your visit.
After reclining on the surgery table, an antiseptic solution is used to paint the scrotum and reduce skin bacteria. The incision area is isolated by sterile towels. The upper or middle of the scrotum will be chosen for the operation site, because the vas is closest to the skin. A local anesthetic is injected into the skin with a fine needle and a slight stinging sensation may be experience. After freezing the skin, a small incision or puncture is made. The vas is identified and pulled up into the defect. Despite the additional anesthetic use in the deeper tissues, you may experience a tug or pulling sensation in the scrotum or groin when the vas is being worked on. You may also experience a dull ache in the mid to lower abdomen. The vas is divided and the ends are sealed in a variety of ways. Some physicians use suture while others will just cauterize the ends. Small bleeding vessels will be cauterized and the divided vas ends are replaced into the scrotum and the skin is allowed to heal on its own or is sutured with self-absorbing suture that will dissolve in a week or two.
A small dressing is placed over the incision or puncture site to absorb oozing and to protect the clothing from stain. A suitable athletic supporter is used to immobilize the scrotum and minimize discomfort. Someone will have to be present to drive you home after a1-2 hour period of observation. The total time of vasectomy varies from 15-45 minutes, depending upon the circumstances.
Dressing
Dressing should be changed when stained or soiled. Small sterile gauze squares are available at any drug store. They can be removed when the dressing is dry or there is no stain which usually occurs within a day or so.
Athletic supporter
The supporter keeps the scrotum from moving in order to reduce the discomfort. It can be worn as long as comfortable.
Bathing
Bathing or shower can start the day after the vasectomy. It is better to shower rather than bathe and to avoid rubbing the incision or puncture with a towel. Use a pat-like maneuver to dry the scrotum.
Healing
The small incision or puncture will heal with a minimal scar and will become almost invisible, especially to others.
Skin separation
Some times the skin will separate due to tissue fluid, oozing blood, or premature release of the skin suture if used. The edges can be pinched together for a period of time to stop any bleeding and help with the healing process.
Bruising
Black and blue discoloration is common because of bleeding of the small vessels within the skin. There is usually no discomfort and the color will fade within a week.
Pain
After the local anesthetic wears off in couple of hours, there may be a mild discomfort, which varies according to each person. This may be treated with simple pain medication every four hours. Shaved or crushed ice in a plastic bag can be placed over the supporter and dressing and can provide relief for hours at a time.
Skin suture
If suture material has been used, they will dissolve within a couple of weeks and need not be removed. Where no skin sutures are used, the skin edges will stick together and heal.
Physical activity
Rest on the day of the vasectomy is recommended. Usually daily activities can be resumed the day after the vasectomy unless vigorous physical activity or exercise is involved. Then the general guideline is to avoid these activities for four to five days.
Swelling
It is ordinary to experience some degree of swelling of the incision after the vasectomy. Usually this swelling subsides within a few days. Shaved or crushed ice in a plastic bag can be placed over the supporter and dressing during the first 24-48 hours can decrease the amount of swelling.
Sexual activities
Sexual activity can begin in a few days when scrotal swelling and tenderness starts to subside. The first few ejaculations may cause a dull ache in the testicles but this general over time disappears. Living sperm still reside in the vas, seminal vesicle and ejaculatory ducts. Until this storehouse is eliminated with multiple ejaculations (>20), contraceptive protection is an absolute requirement; otherwise, a pregnancy can still result. You not considered sterile until two consecutive semen analysis tests show "no sperm".
No operation can be guaranteed perfect and free from complications regardless of the skill and careful technique of the operating physician. Vasectomy is no exception but fortunately, these complications are a few in numbers and relatively minor. You need to be aware of these problems, the consequences and the methods of resolving these problems.
Bleeding
Superficial- Bleeding from the skin edges or just beneath the skin is common and usually stops within several hours. If the skin edges continue to ooze, pinching the bleeding tissue with gauze or applying pressure on the area for several minutes will usually halt the bleeding.
Deep- The loose elastic tissue of the scrotum allows bleeding to expand rapidly. Most of the time the bleeding stops and only a thickened tissue or knot remains. This gradually softens and disappears. Bleeding that does not stop may expand and require a re-opening of the scrotal incision and tying off the bleeder. Fortunately, this occurs only rarely.
Inflammation/infection
Tissue or incision tenderness, redness, and swelling can be related to the reaction caused by the surgery or infection organisms. Despite bathing and pre-vasectomy antiseptic solution, some germs may remain. In addition, germs can be freed at the time when the vas is divided. The site of inflammation can include the deeper scrotal tissue, vas deferens, testis, and epididymis. The degree of inflammation ranges from mild redness, swelling and soreness to discharge draining from the incision or from development of an abscess. Treatment varies from observation without treatment to exploration and drainage. Warm soaks, anti-inflammation medication and antibiotics may be useful. Fortunately, the percentage of the more serious infections causing fever and chills is rare.
Sperm Granuloma
Sperm leakage from the vas deferens during the division or post-vasectomy can result in a tissue reaction called sperm granuloma. It is felt as a knot-like thickening of fibrous tissue at the end of the vas deferens. Most of the time the knot is small in size and of little consequence but some men complain of knot sensitivity, ache in the scrotum, or groin discomfort. If both ends of the vas are joined by the sperm granuloma then there is a chance that living sperm can appear in the semen, resulting in fertility.
Your physician should be consulted if a sperm granuloma results or develops, causes symptoms, or increases in size. Treatment is removal of the sperm granuloma and a repeat vasectomy.
Vasectomy failure, primary and secondary
Primary- If dead or live sperm are noted in the semen after one is normally expected to be sterile, then the cause might be the presence of another vas, which is very rare. Other reasons may include the dividing of a vessel or structure other than the vas deferens or an incomplete division of the vas, which allows it to rejoin. It will be necessary to repeat the vasectomy if this problems continues. Fortunately, this difficulty occurs in a very small percentage of men.
Secondary- When semen analysis after vasectomy indicates a sterile specimen (absence of dead sperm or live sperm) and sperm are discovered at a later date, the likely cause is a gradual rejoining of vas deferens segments. This a rare occurrence irregardless of surgery techniques. Tissue that is interposed between the vas ends at the time of vasectomy is less likely to cause rejoining. Treatment for rejoined vas deferens is a repeat vasectomy.
While a small percentage of complications is unavoidable with any procedure, the key to vasectomy success is your awareness of possible problems, followed by recognition and correction. You and your physician can work together for your mutual satisfaction.
If there is any doubt or questions about this procedure, always consult your physician.
Frequently Asked Questions
What is a vasectomy?
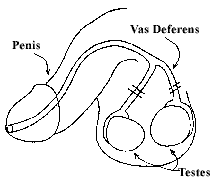
As you probably know already, a vasectomy is a surgical procedure that renders a man sterile. What you may not know are the specifics of the procedure and the period that follows. This literature is designed to give you a better understanding of both, before the surgery takes place. To begin with, you should have some basic knowledge of the anatomy and physiology of the male reproductive system. Sperm cells travel from the testicles through the vas deferens, become part of the seminal fluid (which is produced by the seminal vesicles and the prostate gland), and are ejaculated through the penis. When the surgeon performs a vasectomy, he cuts through the vas deferens extending from each testicle. He then removes a small segment of the vas deferens and ties off the two remaining ends. The object of the procedure is to make it impossible for the sperm to become part of the seminal fluid. Since conception cannot take place in the absence of sperm, a vasectomy results in permanent male sterilization.
Will I be sterile as soon as the operation is over?
No. Contrary to what many people believe, you may not be sterile immediately after the operation. This is because there are some sperm residing above the area where the vas deferens is cut during the procedure. Until all of these sperm cells have been ejaculated, you will still be fertile. In general, it takes several months following vasectomy for sperm to disappear. Patients need to bring a semen sample to the office about 2 months after the surgery. The physician will examine the seminal fluid under a microscope to be sure that no sperm are present. Only when this has been confirmed can you be sure that the surgery has been a success.
Are the effects of the surgery permanent?
Yes. Essentially, once the surgery has been declared successful, you will be permanently sterile. The chances of the two cut ends of the vas deferens being spontaneously rejoined are extremely rare, probably no more than 1 in 200 to 1 in 1,000. For this reason, it is most important that you are completely sure that you want no more children before you consent to the surgery.
Suppose I change my mind later on. Can the operation be reversed?
Your physician can reconnect the two ends of the vas deferens, and once this is done, you may possibly be fertile again. However, after the procedure, called a vas reanastomosis, fertility is restored in fewer than 40% of the patients on whom it is performed. Therefore, you should consider the vasectomy to be an irreversible procedure.
How will the procedure affect my sex life?
Although the vasectomy will make you sterile, it will have no effect whatever on your potency - that is, your ability to have sexual intercourse. In fact, many couples find that their sex life improves after the vasectomy because they no longer have to worry about the surprise of an unwanted pregnancy.
Will I still ejaculate in the normal manner?
Yes. Most of the seminal fluid that the male ejaculates during intercourse is produced by the seminal vesicles and the prostate gland. Only a small amount of the seminal fluid consists of sperm. Therefore, after a vasectomy, ejaculation will take place in the same way as it did before. The only difference is that there will be less fluid ejaculated, and this difference is barely noticeable.
I've heard that the vasectomy can be performed in the physician 's office. Is this true?
This is a matter to be discussed with your physician, and you should follow his recommendation. Although the procedure is relatively uncomplicated and can be performed with minimal difficulty in the physician's office, many physicians find it more convenient to perform the vasectomy in a hospital setting.
Is a vasectomy painful?
As with any operation, no matter how minor, there will be some discomfort associated with it. However, with proper anesthesia, this discomfort will be kept to a minimum. Your physician will discuss the type of anesthesia to be used. As a rule, local anesthesia and some supplemental sedation are all that is required. In some cases, general anesthesia may he needed, but this is a matter to be left to the discretion of your physician.
Are there any complications associated with a vasectomy?
The problems that occur after the operation are usually quite minor. There will be some pain and tenderness in the area where the surgery is performed. There may also be some swelling and discoloration (black and blue marks). Your physician will probably prescribe some medication to keep the post-procedure discomfort to a minimum. As with any surgery, the possibility of an infection is always present. However, this is usually quite rare following a vasectomy. In a very small percentage of patients, a blood vessel inside the scrotum continues to bleed after the operation. If this happens, the scrotum will swell and become very tender. Should you experience this problem, contact your physician. He may have to re-open to tie off the "bleeder". This could require a return to the hospital and the administration of general anesthesia.
Are there any long-term complications?
As far as medical science can determine at this time, there are no long-term complications associated with vasectomy. Recent reports in the lay press have focused attention on scientific studies that raise the question of an increased risk of heart disease or an increased risk of prostate cancer. The current consensus is there is no clear proven risk between vasectomy and other health conditions.
How soon after the operation can I have sexual intercourse?
You may resume your normal sexual activity one week after the surgery. Remember, however, that you may not be sterile until some time after the operation, and therefore you should continue to use some form of birth control until your doctor confirms that all sperm have disappeared from your semen.
What about after the operation. What must I do?
Wear the athletic supporter or suspensory for the first 24-48 hours after the operation. After that you need only wear it if it makes you more comfortable. Do not engage in any strenuous physical activity for the first week, and work your way back to your normal routine over a period of about one to two weeks. You may shower on the day after the surgery. Just be sure that you wash the scrotal area gently, and rinse with warm water. When you dry the scrotum, do so by blotting the water with a soft towel. If your physician uses stitches to close the incisions, they will dissolve themselves and you will not have to return to have them removed. However, because the incisions are so small, many physicians do not use stitches. In such cases, there may be a slight discharge from either or both of the incision sites. This need not concern you. Simply place a small sponge or gauze pad over the incision, replacing it on an as-needed basis, until the wound is completely healed. Even with such a discharge, you may still shower each day.
One final word..
Discuss any questions you have about the procedure with your physician before the surgery takes place. Follow all his instructions completely. Be as certain as you possibly can be that you want no more children before you consent to the surgery.
[ back to top ]